Skin cancer is characterized as the abnormal growth of skin cells. It is more common than you may have thought as one in every three cancers diagnosed is a skin cancer, as reported by the World Health Organization. It is also considered as the most common type of malignancy in the Caucasian population, with Basal cell carcinoma being the most common cancer in Caucasians, Hispanics, Chinese Asians and Japanese. For Asians, skin cancer represents 2 to 4% of all cancers. Skin cancer is often found in areas that are frequently exposed to sunlight (UV radiation), although some people can suffer from skin cancer all over the world, due to the varying risk factors.
There are two main types of skin cancer, melanoma and non-melanoma. Non-melanoma refers to skin cancer that slowly develops in the upper layers of the skin. The most common non-melanoma skin cancers are basal cell carcinoma and squamous cell carcinoma that account for 90% of skin cancers. While the more aggressive skin cancer, melanoma, accounts for 4% of skin cancers.

Myth: Sun damage is not possible on a cloudy or cool day.
Fact: Damage to the skin is caused by UV radiation, not the temperature. UV radiation can penetrate some clouds and in some cases can be more intense due to the reflection.
The incidence of skin cancer worldwide is increasing as depleted ozone levels affect the protective filter function of the atmosphere, allowing more solar UV radiation to reach the Earth's surface. It is estimated that a 10 per cent decrease in ozone levels will result in an additional 300,000 non-melanoma and 4,500 melanoma skin cancer cases. Beaches from Phuket to Bali register some of the highest UV radiation levels in the world. Other factors that may increase the risk of skin cancer include exposure to toxic substances and compromised immune system.
Basal cell carcinoma
Basal cell carcinoma, also known as rodent ulcer, usually occurs in areas with prolonged exposure to sunlight such as the neck and face. It is presented as a small raised area that may enlarge slowly over months or years. It will develop into a shiny pink or pearly-white lump with a translucent or waxy appearance. It can also manifest as a red, scaly patch. Often mistaken as pimples, recurrent crusting or bleeding of the basal cell carcinoma is common.
Squamous cell carcinoma
Squamous cell skin cancer also occurs in sun-exposed areas of skin. It is marked by the appearance of a firm pink lump with rough or crusted, flaky surface. The lump is often painful to touch, bleeds easily and may develop into an ulcer.
Malignant melanoma
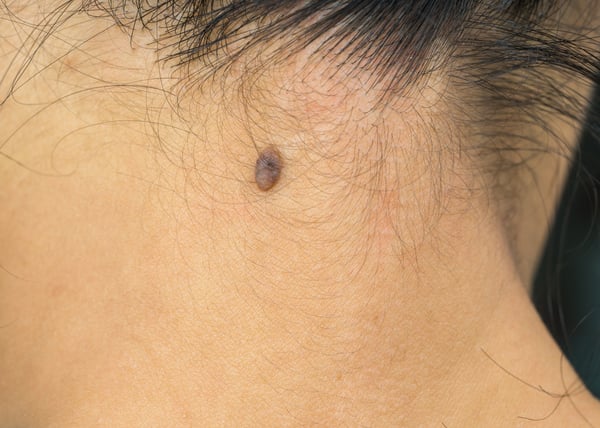
Malignant melanoma, also known as melanoma is an aggressive skin cancer that arises from the melanocytes, the cells that control skin pigmentation. Malignant melanoma, although represents only 4% of skin cancer cases, is responsible for 65% of all skin cancer-related deaths. Melanoma may occur in any area, regardless of sun exposure. It may begin as dark brown or flat black spot or develop from a pre-existing mole. The ABCDE rule can serve as useful warning signals for the signs and symptoms of most melanomas.
- Asymmetry: one half of the mole does not match the other half
- Border irregularity: the edges are ragged, notched, or blurred
- Colour: the pigmentation is non-uniform, with variable degrees of tan, brown, or black
- Diameter: diameter greater than 6 mm; about the size of a pencil eraser
- Evolution, elevation, and/or enlargement of a lesion.
(send%20to%20client).jpg?width=2619&name=16%20Jan%20Skin%20Cancer%20(Infographic)(send%20to%20client).jpg)
Myth: If you are wearing a sunscreen with SPF50+ you can stay in the sun for more time.
Fact: No, sunscreen should never be used to extend this amount of time you exposure your skin to the sun. In fact, SPF50 only gives you marginally better protection from UVB radiation. SPF30 filters 96.7% of UV radiation, compared to 98% of UV.
Not all changes in your skin are signs of cancer but visit your doctor as soon as possible if you notice any concerning change. Dermatological consultation usually involves examination of the skin while suspected skin lesion may be subjected to biopsy for further assessment. Early detection and treatment of melanoma might reduce death risk, while early detection and treatment of non-melanoma skin cancer might prevent major disfigurement.
Although mostly suspected in older, fair-skinned individuals, some studies have shown an increase in melanoma incidence among young individuals, aged 35 to 65 years. Risk factors such as immune suppression, gender, skin tone and age can all affect your likelihood of developing skin cancer. The American Academy of Dermatology recommends that those at highest risk, having a strong family history of melanoma and multiple atypical moles, should perform frequent self-examination and seek professional evaluation of the skin at least once per year.
Compared with other parts of the world, Thailand is among the low incidence-rate countries for malignant melanoma. As skin cancer prevalence is not as high as in Caucasian, availability of expert dermatologist on skin cancer in the local hospitals may be limited. Our guide to international hospitals in Bangkok may help you in choosing the best hospital available. Samitivej Hospital, for example, provides a comprehensive skin cancer screening program. If left untreated, skin cancer can spread to other parts of the body and can increase the incidences of developing other types of cancer.
As proper screening and diagnosis in a high-quality facility may be costly, a comprehensive health insurance can ensure a better access to all the available options. It will also provide coverage to cover the relevant medical tests that you should do as you aged. Our guide in choosing the best health insurance in Thailand can help you to search for one that suits you.
Myth: You can’t get burnt through a car window.
Fact: Untinted glass used in car windows can reduce, but not entirely block the transmission of UV radiation.
The Bottom Line
Despite the risk of skin cancer associated with sun exposure, healthy sun exposure is actually highly beneficial for vitamin D formation and is associated with a reduced risk of melanoma, hypertension, and numerous internal cancers. In fact, it has long been observed that outdoor workers have a lower incidence of melanoma than indoor workers.
In contrast, sunburns which indicate excessive exposure to sunlight are associated with a double risk of melanoma. A study shows that women who had five or more blistering sunburns between the ages of 15 and 20, compared to those that had none, have a higher risk of melanoma by 80%.

Hence, prevention should be practised through proper protection from the ultraviolet radiation of the sun.
-
Avoid the sun during hours of high ultraviolet radiation - 10:00 to 16:00.
-
Clothing (made of thick material) that covers skin exposed to the sun
-
Use sunscreen (above SPF of 30 or more) that blocks both UVA and UVB radiation to all exposed skin
-
Apply sunscreen at least 30 minutes before exposure to the sun and reapply it every 2 hours
-
Moisturize your skin adequately to prevent degenerative damage to sun exposure
-
Using hats and wrap around sunglasses
-
Keep young children, especially babies younger than 6 months shield from the sun
-
Tanning bed should also be avoided as it can pose a risk of sunburn as well
- Ensure you have comprehensive health insurance that cover preventative skin check ups.
As the famous Australian Cancer Council health campaign goes:
Slip, Slop, Slap!
.png)